overview
Head injuries are dangerous and can cause serious medical problems. A subdural hematoma is due to a severe trauma to the head. It can lead to coma or death to the patient. This blog is a comprehensive guide to subdural hematoma, its symptoms, causes, and available treatment options.
What is subdural hematoma?
When blood collects outside the brain, it is called a subdural hematoma. Blood collects between the layers of tissue surrounding the brain. Dura mater is the term for the top layer. Bleeding occurs between the dura and the next layer, the arachnoid. This is usually due to a severe head injury, which can cause life-threatening bleeding and increased pressure on the brain. Some stop on their own, while others require surgical drainage of the accumulated blood.
In a subdural hematoma, the bleeding is outside the brain under the skull. But when the blood pools, the pressure on the brain increases. Symptoms are due to pressure on the brain. A subdural hematoma can lead to unconsciousness and even death when the pressure within the skull becomes extreme.
What types of subdural hematomas are there?
Doctors classify subdural hematomas into three types, depending on how quickly they form, how much blood bleeds, and how much harm the bleeding does:
- Acute subdural hematoma: This type of subdural hematoma is the most dangerous. Severe symptoms develop soon after a brain injury, often within minutes to hours. Blood pools and pressure on the brain rises rapidly. Without prompt diagnosis and treatment, people can faint, become paralyzed, or even die.
- Subacute subdural hematoma: Symptoms may appear hours, days, or even weeks after a head injury.
- chronic subdural hematoma: Older people are more likely to develop this type of hematoma. Slow bleeding can take weeks or months before symptoms appear. A chronic subdural hematoma can result from a minor head injury. Older people may not remember how they suffered a head injury because the onset of symptoms is delayed. In addition, changes can be so subtle and slow that family members may not notice any symptoms.
What are the symptoms of subdural hematoma?
Bleeding rate primarily affects the symptoms of subdural hematoma.rear brain injury, a person may appear normal for several days, but gradually begins to lose consciousness. This is due to the slow bleeding rate. Bleeding may last for two weeks and he may not show any symptoms. However, when a subdural hematoma is caused by sudden heavy bleeding from a head injury, the victim quickly loses consciousness or coma.
Signs and symptoms of a subdural hematoma include behavior changes, confusion, dizziness, weakness, lethargy, nausea, diarrhea,sleepiness, headache Also seizure.
These symptoms vary depending on factors such as age, health problems, and size of the subdural hematoma, which can affect how the body responds. Older people are more likely to develop slow-growing subdural hematomas. It can cause apathy and subtle personality changes.
Typical symptoms include:
- Perceptual and constant headache.With acute subdural hematoma, headache is generally severe
- confusion and drowsiness
- vomiting
- Speech and visual changes
- Lightheadedness, loss of balance, difficulty walking
- amnesiadisorientation, and personality changes, especially the elderly who suffer from subdural hematoma
- A baby with a big head.Baby’s soft skull can grow as blood accumulates
Continued bleeding worsens symptoms and puts pressure on the brain. Symptoms include:
- paralysis
- Loss of consciousness and coma
- breathing problems
When do you want to see a doctor?
If a person experiences these symptoms, immediately visit a healthcare provider and seek help.
What causes subdural hematoma?
A head injury, usually from a fall, car accident, or assault, causes a subdural hematoma. A quick blow to the skull cuts blood vessels along the surface of the brain. The medical term for this condition is acute subdural hematoma.
Subdural hematomas tend to form in patients who are taking blood thinners or who have a bleeding condition. People who bleed easily can develop a subdural hematoma even after a minor head injury.
Chronic subdural hematoma is more common in the elderly due to shrinkage of the brain, which makes small veins more tense and prone to tearing.
Who is at risk of developing a subdural hematoma?
Anyone can experience a subdural hematoma from a head injury, but some people are prone to subdural hematoma. It is common in the following people.
- senior citizen: As a person ages, the brain shrinks within the skull, creating a large gap between the skull and the brain.The large gap allows small veins in the membrane between the skull and the brain to stretch. In addition, stretched and thinned veins are most likely to rupture in minor head injuries, such as falling from a chair.
- Contact information for sports representatives: Athletes who participate in high-impact sports such as soccer are at increased risk of developing a subdural hematoma.
- People taking blood thinners: Anticoagulants reduce the clotting process or prevent blood from clotting altogether. Failure of the blood to clot causes severe, long-term bleeding after minor injuries.
- Hemophiliacs: person who has hemophilia Known as a hemophiliac. Hemophilia is a genetic disorder in which the blood does not clot. People with hemophilia are at increased risk of uncontrolled bleeding after trauma.
- People with Alcoholics and Alcohol Use Disorders: Excessive drinking over time can my liver hurtsA damaged liver cannot produce enough protein to help blood clot. Therefore, the risk of uncontrolled bleeding increases.
- Baby: Babies lack strong neck muscles to protect themselves from head trauma. Therefore, if a person shakes the baby violently, a subdural hematoma can occur.such injuries are called shaken baby syndrome.
What tools are used to diagnose subdural hematoma?
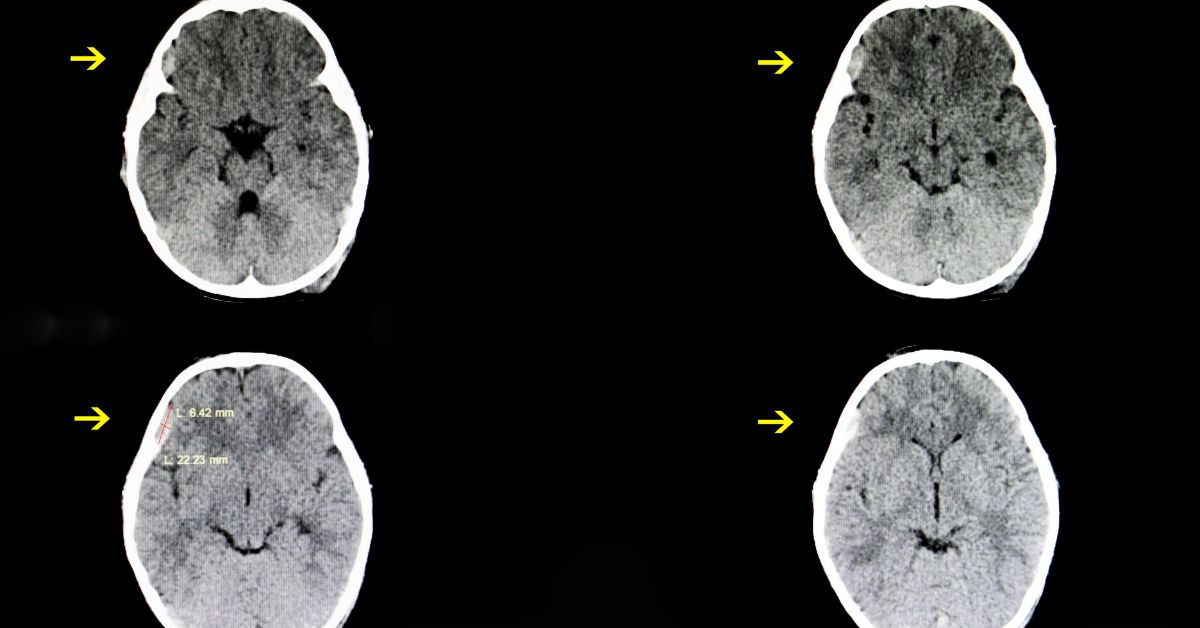
After a head injury, patients usually have a computed tomography (CT) scan or magnetic resonance imaging (MRI scan). These tests produce pictures of the inside of the skull and usually identify subdural hematomas. CT is faster and more accessible, but MRI can detect subdural hematomas more effectively. Angiography is rarely used to identify subdural hematomas.
What are the treatment options for subdural hematoma?
The severity of the subdural hematoma determines treatment options. The only recommended treatment for mild subdural hematoma with moderate symptoms is continued observation. Repeated imaging of the head is common to monitor the progression of a subdural hematoma.
For more severe or acute subdural hematomas, surgery is needed to relieve pressure on the brain. Doctors use a variety of surgical procedures to treat subdural hematomas.
- Burr hole drilling: A hole is made in the skull over the site of the subdural hematoma. Helps suck excess blood.
- Craniotomy: In this procedure, doctors remove a large portion of the skull to relieve pressure. When the pressure drops, the resected skull is replaced.
- Craniectomy: Here, doctors remove part of the skull for a long time. This procedure helps the injured brain expand and expand without long-term damage. Subdural hematomas are rarely treated with craniectomy.
Serious illness requires the use of machines to keep people with severe subdural hematoma breathing and other forms of life support. If a person has bleeding problems or is taking blood thinners, improvement of blood clotting should be done. If so, blood thinners should be discontinued. Additional drugs may be needed to control attacks, reduce pressure in the brain, and relieve swelling.
What are the complications of subdural hematoma?
Severe consequences of some subdural hematomas can result in coma or even death. It can occur if a hematoma is left untreated. Potential issues are:
- Brain Hernia: A subdural hematoma is when the brain pushes tissue out of its normal place. This can lead to death.
- bleeding: During the healing phase of the initial bleeding, older people are more likely to experience additional bleeding, especially if they have suffered a head injury.
- Seizures: Patients may still experience seizures even though the hematoma has been repaired.
Conclusion
A subdural hematoma is a potentially fatal condition. The prognosis of health after subdural hematoma depends on the age of the patient, the severity of the head injury, and how quickly the patient was treated. Younger people are more likely to survive. After a subdural hematoma, older people are at increased risk of experiencing another brain hemorrhage. Therefore, seek appropriate medical help at the appropriate time.
Frequently Asked Questions (FAQ)
How to prevent subdural hematoma?
Prevention is better than cure. Therefore, use safety belts and helmets when riding in vehicles to protect your head from injury. Always use protective gear when playing high-impact contact sports. Avoid places where the elderly can slip.
Who is at increased risk of getting a subdural hematoma?
Older people, infants, people taking blood thinners, athletes, and people with hemophilia are at increased risk of developing a subdural hematoma.
Can subdural hematoma be treated with medicine?
In less severe cases, drugs may cure a subdural hematoma.
https://healthlibrary.askapollo.com/subdural-hematoma-types-symptoms-causes-treatment/ Types, Symptoms, Causes, Treatment and Diagnosis